 89 year old male with PMH of hypertension, stage 3 chronic kidney disease with chief complaint of shortness of breath. Several days ago patient had a laminectomy for radicular pain. He was doing fine post-operatively and began to develop gradual shortness of breath. He had no complaints of chest pain, nausea/vomiting, fevers, diaphoresis, but did have some weakness. There were no prior ECGs for comparison.
89 year old male with PMH of hypertension, stage 3 chronic kidney disease with chief complaint of shortness of breath. Several days ago patient had a laminectomy for radicular pain. He was doing fine post-operatively and began to develop gradual shortness of breath. He had no complaints of chest pain, nausea/vomiting, fevers, diaphoresis, but did have some weakness. There were no prior ECGs for comparison.
BP: 98/48 HR: 103 RR: 18 O2 on RA: 94% Temp: 38.6
JVD to the angle of the mandible
Bibasilar Crackles
Sinus Tachycardia
Bilateral lower extremity pitting edema
Labs: Na 125, K+ 4.2, Creatinine 2, BNP > 2500
ECG from triage is shown…
Before reading on, try to come up with your own interpretation of this ECG before moving on to the final impression
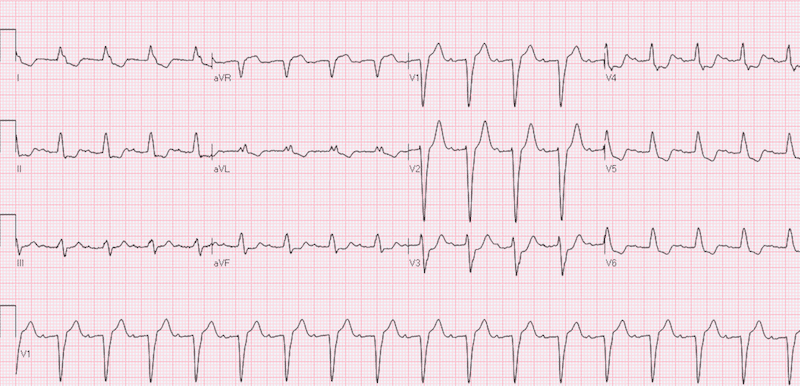
Rate: 103
Rhythm: Normal sinus Rhythm, 1st degree AV Block
Axis: Normal Axis
QRS: Left bundle branch block (LBBB)
ST/T Waves: Flattened ST depression in Leads II, III, aVF and V5 – V6, J point elevation in leads V2 – V3, V3 concordant ST depression
Final ECG Interpretation: LBBB with concordant ST depression in lead V3
Putting all this together we have a patient with new onset congestive heart failure based on physical exam, and based on the fact that there is no old ECG it is unknown if this LBBB is new, but there is concordant ST depression in lead V3. In this case cath lab should be activated.
What is the ACC/AHA STEMI guideline recommendations for LBBB and STEMI?
The 1996 and 2004 ACC/AHA STEMI guidelines recommended emergent repercussion therapy including fibrinolytics or primary percutaneous coronary intervention (PCI) in patients with symptoms compatible with STEMI and new or presumably new LBBB if these symptoms arose in the prior 12 hours (Class I Indication)
The 2012 European Society of Cardiology STEMI guidelines also recommend early PCI or fibrinolytics in patients with a clinical presentation of STEMI and new or presumably new LBBB if symptoms arose in the prior 12 hours (Class Ia Indication)
The 2013 ACC/AHA STEMI guidelines changed previous recommendations for patients with suspected ischemia and new or presumably new LBBB should not be treated as a STEMI equivalent
What is the role of the Sgarbossa criteria and modified Sgarbossa criteria in patients with LBBB?
- For a complete explanation checkout this post from REBEL EM, Modified Sgarbossa Criteria: Ready for Primetime?
- The bottom line of that post:
- Suspected Acute Myocardial Infarction (AMI) + LBBB needs to have emergent primary PCI or fibrinolysis IF:
- Hemodynamic instability or acute heart failure (Validated)
- Sgarbossa score ≥ 3 (Validated)
- ST/S ratio < -0.25 (Proposed, NOT Validated)
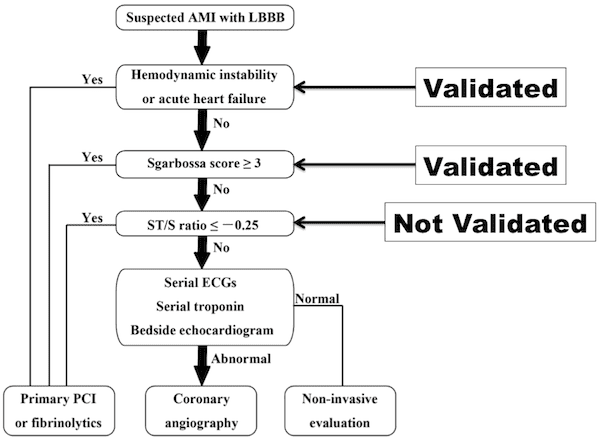
Image modified from:[cite source=”pubmed”]24016487[/cite]
Conclusion to the case:
- This patient has an ECG with LBBB and hemodynamic instability with signs of acute congestive heart failure which according to the above algorithm requires primary PCI or fibrinolysis
- It was decided to activate the cath lab, and patient was found to have a 100% RCA lesion, and 80% LM stenosis.
- Sensitive Troponin I showed an initial Troponin of 45 before cath was performed
Take Home Point:
Patients with LBBB, concordant changes in any one lead (i.e. Sgarbossa Criteria ≥3), and signs of hemodynamic instability or congestive heart failure, STEMI is the diagnosis until cardiac catheterization proves otherwise



