 Background: POCUS has been touted as the stethoscope 2.0, a true game changer in patient care. There is no patient population that this statement should hold more true for, than in patients with undifferentiated shock (SBP <100mmHg or SI > 1). Everyone has a story about how ultrasound changed their management or even saved a patient’s life. Unfortunately, the plural of anecdote is not data. To date, there have not been any prospective randomized controlled trials examining POCUS outcomes on survival in this population. Enter the Sonography in Hypotension and Cardiac Arrest in the Emergency Department (SHoC-ED) trial.
Background: POCUS has been touted as the stethoscope 2.0, a true game changer in patient care. There is no patient population that this statement should hold more true for, than in patients with undifferentiated shock (SBP <100mmHg or SI > 1). Everyone has a story about how ultrasound changed their management or even saved a patient’s life. Unfortunately, the plural of anecdote is not data. To date, there have not been any prospective randomized controlled trials examining POCUS outcomes on survival in this population. Enter the Sonography in Hypotension and Cardiac Arrest in the Emergency Department (SHoC-ED) trial.
REBEL Cast Episode 58 – Would you be SHoC-ED if POCUS did not Improve Clinical Outcomes in Patients with Undifferentiated Shock?
Click here for Direct Download of Podcast
What They Did: This was an international, multicenter, randomized controlled trial from 6 centers (3 centers in North America and 3 centers in South Africa) of patients with undifferentiated hypotension (SBP <100mmHg or Shock Index > 1) in the ED randomized to an early POCUS protocol + standard care vs standard care without POCUS evaluating survival and clinical outcomes.
POCUS Protocols Used (Combination of):
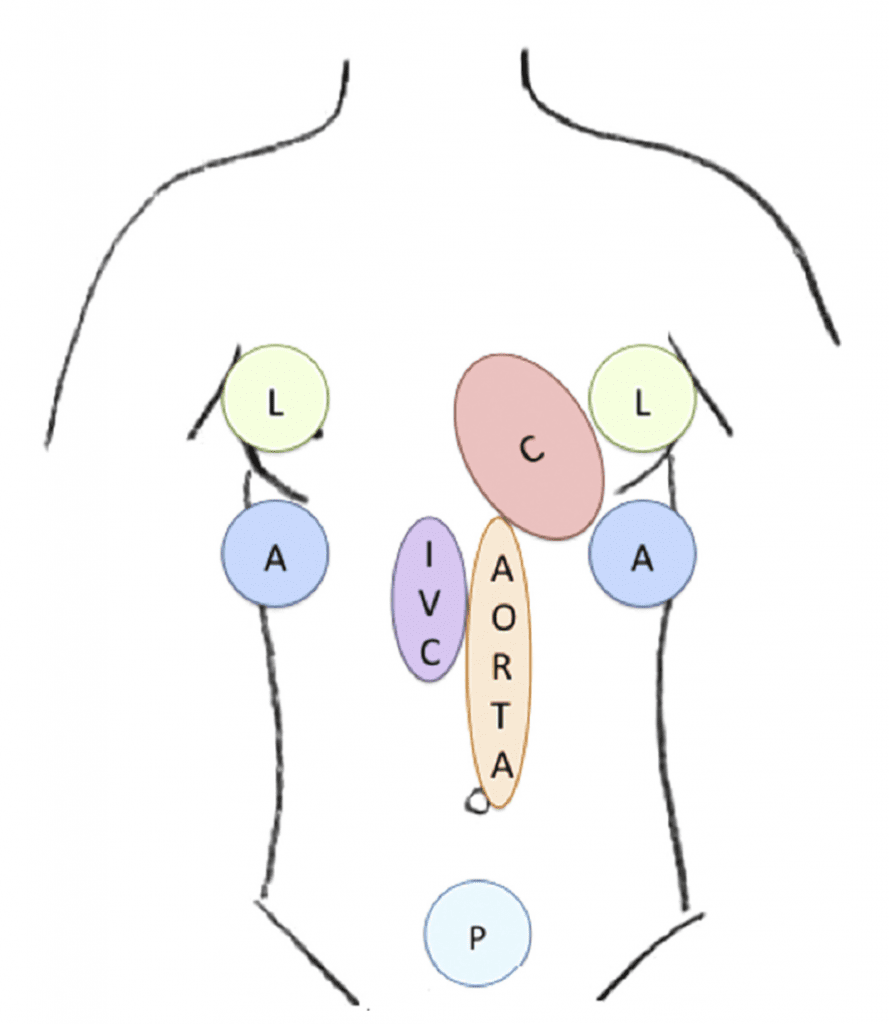
- Abdominal and Cardiac Evaluation with sonography in Shock (ACES)
- Rapid Ultrasound for Shock and Hypotension (RUSH)
Outcomes:
- Primary: Survival at 30d or hospital discharge
- Secondary:
- Initial treatment (inotrope and IV fluid administration)
- Investigations (rates of CT use)
- Admissions (Hospital and ICU)
- Length of stay (Hospital and ICU)
Inclusion:
- Sustained SBP <100mmHg
- Shock index > 1.0 + SBP < 120mmHg
- ≥19 years of age
Exclusion:
- Pregnant
- Necessity of cardiopulmonary resuscitation or other advanced cardiac life support interventions (i.e. defibrillation, emergency pacing, insertion of ventricular assist device)
- History of significant trauma in the past 24 hours
- 12 lead ECG diagnostic of acute myocardial infarction
- Obvious cause for hypotension or shock
- Previously known diagnosis from another hospital (for transferred patients)
- A vagal episode as cause of hypotension
- Low blood pressure considered to be non-pathologic (normal variant or other)
Results:
- Follow up completed for 270 out of 273 patients
- Most common category of shock = non-cardiogenic (87.6%)
- Most common diagnosis = occult sepsis (52%)
- Survival at 30d or Hospital Discharge:
- Early POCUS + Standard Care: 76.5%
- Standard Care Without POCUS: 76.1%
- 95% CI: -10.2% – 11%
- Survival at 30d or Hospital Discharge in North America:
- Early POCUS + Standard Care: 85.4%
- Standard Care Without POCUS: 81.8%
- 95% CI -8.1% – 15.3%
- Survival at 30d or Hospital Discharge in South Africa:
- Early POCUS + Standard Care: 59.6%
- Standard Care Without POCUS: 65.2%
- 95% CI: -15.2% – 26.0%
- No differences in rates of CT scanning, inotrope use, intravenous fluid use, ICU admissions, or total length of stay
Strengths:
- This study asks an important clinical question about the use of POCUS in shock patients and evaluates patient oriented outcomes
- Several North American investigating physicians visited South Africa, and vice versa, to confirm that competency standards were comparable at all locations
- Categories of shock and diagnoses were established by independent chart review by 2 clinicians, blinded to the initial sonographer, POCUS findings, initial and revised diagnoses
- Baseline demographics and vital signs were similar between groups
Limitations:
- Exclusion of “clear cause of shock.” Would have been useful information to know how many times there was a “clear cause” and then POCUS changed that diagnosis
- This was a convenience sample of eligible patients only when appropriately trained staff were immediately available in the ED. As we have discussed before on the blog, the issue with convenience sampling is that the sample represented in the study is not representative of an entire population. How do we know that the patients not enrolled that would have been eligible would not have altered the results of the study?
- The definition of sustained hypotension of <100mmHg is not clear from the paper.Is this 2 minutes, 5 minutes, 30 minutes, etc?
- POCUS scans were performed within the first 60 minutes of the patient visit, and all findings were recorded immediately after each step. In both groups physicians performed a secondary clinical assessment and recorded their revised impressions at 60 minutes. POCUS is typically done within minutes of arrival in clinical practice, so 60 minutes of the wrong treatment is not going to result in beneficial outcomes.
- Although the physicians using POCUS are trained in POCUS at the 6 different sites there was no inter-observer evaluation to see if what was read on the ultrasound would be read by someone else the same way
- This was a very small study. A huge issue with this study was that 400 patients were needed to provide an 80% power to detect a reduction in mortality of 10% assuming a mortality rate of 30% in the control group. This study only enrolled just over half of these numbers (study was stopped early due to slow recruitment and futility), and the mortality in the control group was <30%, making it impossible to determine if POCUS compared to standard care alone has no effect based on this study alone.
- A 10% mortality reduction with any intervention is extremely bold. 5% or less may have been a better goal and may have been clinically relevant
- The most common diagnosis was occult sepsis, which POCUS would not be able to distinguish from standard care as there is a spectrum of non-specific POCUS findings that could potentially be seen on POCUS.
- Huge exclusion list, after the study was designed, removed patients that might have received benefits from POCUS. Essentially, over the course of the study, people used POCUS more often so certain groups were removed (i.e. AAA, STEMI, Trauma, Ectopic Pregnancy).
Discussion:
- There was an extremely low rate of diagnoses where POCUS would have been helpful:
- AAA/Aortic Dissection – 2 patients
- VTE – 7 patients
- LV Dysfunction/MI – 22 patients
- Cardiac Tamponade/Effusion – 2 patients
- There are two things this study tells me that are important:
- There is no evidence of harm with POCUS protocols in shock and we should continue to use them as needed in patient management in conjunction with getting a good history and doing a good physical exam
- The majority of undifferentiated shock patients were occult sepsis. Keep this high on your radar as you are evaluating these patients
Author Conclusion:“To our knowledge, this is the first randomized controlled trial to compare point-of-care ultrasonography to standard care without point-of-care ultrasonography in undifferentiated hypotensive ED patients. We did not find any benefits for survival, length of stay, rates of CT scanning, inotrope use, or fluid administration. The addition of point-of care ultrasonography protocol to standard care may not translate into a survival benefit in this group.”
Clinical Take Home Point: The most common diagnosis (≈50%) of patients was occult sepsis. There are no specific POCUS findings that would help differentiate these patients from standard care
- The study needed 400 patients with a baseline mortality rate of 30%. Neither were met, so it is impossible to say from this study if POCUS, has no effect, compared to standard care alone
- Huge exclusion list, including AAA, STEMI, Ectopic Pregnancy, and Trauma which excludes patients who might have received benefits from POCUS
- Lastly, THIS STUDY SHOULD NOT CHANGE PRACTICE. POCUS continues to be a powerful tool in differentiation of the cause of shock and has a huge potential to change patient care
Expert Peer Review:
Haney Mallemat, MD
Emergency Medicine, Internal Medicine, and Critical Care Boarded
Cooper Medical School of Rowan University
Camden, NJ
Twitter: @CriticalCareNow
Keynotable: Learn how to give powerful presentations
Resuscitation Leadership Academy (RLA): Yearlong fellowship for those who want to do more resus and critical care but just don’t have the time to do an actual critical care fellowship or leave where they are at
“Think of diagnosing critically ill patients with your physical exam as trying to find your way around a pitch dark room”, a mentor once told me. “You could stumble around in that dark room and do a physical exam…you’ll feel for familiar items and listen for familiar sounds, but you’re never completely sure of what is truly in front of you. Wouldn’t you rather have a flashlight to look around that dark room? Ultrasound is your flashlight in critically-ill patient…it literally let’s you see things that your physical exam cannot” This interaction resonated with me as a critical care fellow and it is something that I still hold true today in my clinical practice.
With the benefits of ultrasound obvious to me, I was certain that the SHoC-ED trial would demonstrate without a doubt that ultrasound would positively change the outcome for patients with undifferentiated shock when compared to clinical care without the use of ultrasound. However, the authors’ conclusions initially “SHoC-ED” me (pun intended); there was no difference in 30 day survival, no difference in the use of inotropes, no difference in ICU admissions or length of stay and no difference in the rates of CT scanning. How can the omission of ultrasound for critically ill patients not lead to any meaningful patient differences? A deeper look at this study, however, revealed that the devil is in the details.
The authors’ conclusion is that ultrasound is not helpful for patients who have undifferentiated shock, but the question is when is a patient labeled “undifferentiated”? Here are a few points to consider:
- Patients in the study were excluded if their ECG demonstrated STEMI and may have also had cardiogenic shock; if you did not perform a screening an ECG, the ECHO would likely demonstrate abnormality that may have lead to the diagnosis
- Pregnant patients were excluded but perhaps females with ectopic pregnancies and hemorrhagic shock also were excluded. Without a screening pregnancy test, perhaps hemorrhagic shock would have been the diagnosis and have lead to a faster diagnosis.
- Any patients with an obvious cause for shock were also excluded; my question is, what level of clinican makes this assessment of “obvious”? Perhaps the diagnosis was obvious to a skilled senior-level clinician but maybe this would not have been so obvious to a junior-level clinician? Perhaps this is where ultrasound has the most benefits.
The study design is my next major issues. First, it is hard to believe that the authors could not enroll their goal of 400 patients and had to stop the study early. 400 patients with undifferentiated shock seems recruitable in in six centers over the span of four years. With so few patients, however, I do not think a valid conclusion can be made. My second issue is that they were looking for a large reduction in mortality (i.e., 10%); perhaps if they reduced their threshold for a mortality difference they may have found an effect. The next issue is that more than half of the patients with “undifferentiated” shock actually had occult sepsis. Ultrasound probably makes little mortality difference in this population, yet these patients accounted for most of the patients in the study. This could dilute the beneficial effects of ultrasound in undifferentiated patients withoutoccult sepsis. My final issue, and this is my biggest concern, is that there was no standardized algorithm for how clinicians performing the ultrasound used all the information from the ultrasound evaluation to form a cohesive clinical impression for a patient. Could there have been enough clinical variation in interpretation of the ultrasounds which lead to discordant results? Without a standardized algorithm for interpreting the data acquired, I am not sure that we can accept the results of this study as conclusive. A better design would have had an algorithmic decision tree which all the clinicians used to come to a standard agreement on treatment plan.
I appreciate the authors valiant attempt to question whether ultrasound positively affects patients with undifferentiated shock, however I will not change my practice based on this single study. The questions raised about the study design, the lack of enrollment, the lack of a unifying algorithm to standardize interpretations as well as the prior studies which have all positively demonstrated the benefits to ultrasound, all overshadow the authors’ conclusions. When I walk into a dark room I use a flashlight to illuminate all the obstacles that are in my path. When I am resuscitating my critically ill patients, I use the ultrasound to illuminate my patient’s physiology so I am aware of everything (good and bad) that is in the path of my patient.
References:
- Atkinson PR et al. Does Point-of-Care Ultrasonography Improve Clinical Outcomes in Emergency Department Patients With Undifferentiated Hypotension? An International Randomized controlled Trial From the SHoC-ED Investigators. Ann Emerg Med 2018. PMID: 29866583
For More on This Topic Checkout:
Según Olusanya at The Bottom Line: SHOC-ED
Post Peer Reviewed By: Anand Swaminathan, MD (Twitter: @EMSwami)





