
The article attempting to answer this question is currently in press, entitled “The Influence of Arm Positioning on Ultrasonic Visualization of the Subclavian Vein: An Anatomical Ultrasound Study in Healthy Volunteers” (Anesth Analg 2016).
What They Did:
- Anatomic ultrasound study of healthy, nonpregnant volunteers aged 18-50 (n=50)
- Excluded those with history of local surgery or trauma or arm deep venous thrombosis
- One anesthetist obtained all images. Second, blinded ultrasound vascular expert made all measurements
Ultrasound Technique:
- All measurements were performed with the patient in a supine position, on the right side only, with a 7.5 MHz linear probe
- Probes were placed parallel to the clavicle in the infraclavicular position
- Ultrasound images obtained in two arm positions
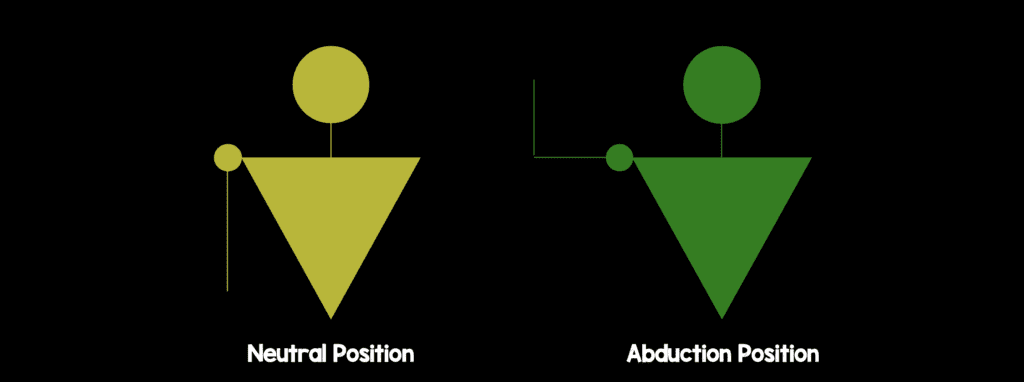
- Arm in neutral position (by the patient’s side)
- Arm in 90° abduction, 90° flexion, and 90° external rotation
Outcomes:
- Cross-sectional area of the subclavian vein in neutral position compared to the abducted position
- Also measured the minimal distance between the vein to the skin, adjacent subclavian artery, and pleura
Results:
- Abducted arm position increased cross-sectional area of the vein in 75% of volunteers (difference of 36 ± 75 mm2, p=0.001)
- Abducted arm position increased cross-sectional area of the vein by ≥50% in at least 27% of volunteers
- Depth of the vein was reduced in the abducted position by a difference of -2 ± 4 mm (p<0.001)
- There was no difference in the distances to the subclavian artery or pleura
Limitations:
- Anatomic study only, no attempts at venipuncture
- Healthy volunteers may differ from critically ill patients (i.e. mechanically ventilated)
- No obese patients were included
- A specific device was used to keep the arm in the abducted position
- Only the right subclavian vein was study (“this study cannot exclude different conclusions for the left side”)
Strengths:
- A 2nd independent ultrasound expert, who was blinded to the arm position and the order of the images performed all measurements
This study, although small, provides some intriguing results. If a simple maneuver like arm positioning can make a significant difference in ultrasound visualization of the subclavian vein, theoretically, complications and failure rates of ultrasound guided subclavian venipuncture could be reduced. A follow up study in critically ill patients using the left side with associated venipuncture would be ideal to cement this maneuver into clinical practice.
Clinical Bottom Line:
During placement of a subclavian central venous catheter, placing the ipsilateral arm in 90° abduction, 90° flexion, and 90° external rotation can increase the cross-sectional area of the vein. This may assist in ultrasound-guided placement of the line, thereby reducing failure and complication rates, but external validation studies with clinically important and patient oriented outcomes are still needed before adopting this technique.
References:
- Sadek M, et al. The Influence of Arm Positioning on Ultrasonic Visualization of the Subclavian Vein: An Anatomical Ultrasound Study in Healthy Volunteers. Anesth Analg 2016. [epub ahead of print]. PMID: 27149016
- Parienti JJet al; 3 SITES Study Group. Intravascular Complications of Central Venous Catheterization by Insertion Site. NEJM 2015;373:1220–9. PMID: 26398070
Post Peer Reviewed By: Salim Rezaie (Twitter: @srrezaie)



