 Lumbar puncture is a procedure that is commonly performed in the emergency department (ED) for both diagnostic and therapeutic reasons. Post lumbar puncture (LP) headache is one of the most common complications from LPs (6 – 36% incidence) and is essentially a clinical diagnosis based on a history of a dural puncture and the postural nature of the headache with associated symptoms. Additionally, post LP headaches that are left untreated can cause impaired ability to perform activities of daily living and there are case reports of subdural hematoma, herniation, and death. In terms of the prevention and treatment of post-LP headaches, both are equally important in management. Following, is a discussion of which techniques and preventative measures are evidence based and which are not.
Lumbar puncture is a procedure that is commonly performed in the emergency department (ED) for both diagnostic and therapeutic reasons. Post lumbar puncture (LP) headache is one of the most common complications from LPs (6 – 36% incidence) and is essentially a clinical diagnosis based on a history of a dural puncture and the postural nature of the headache with associated symptoms. Additionally, post LP headaches that are left untreated can cause impaired ability to perform activities of daily living and there are case reports of subdural hematoma, herniation, and death. In terms of the prevention and treatment of post-LP headaches, both are equally important in management. Following, is a discussion of which techniques and preventative measures are evidence based and which are not.
What is the pathophysiology behind post lumbar puncture headaches? [1]
There are two mechanisms which we believe are the cause of post LP headaches:
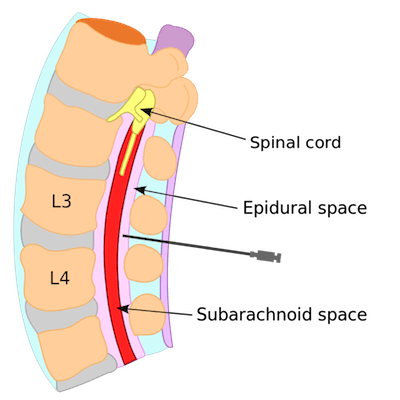 LPs are a traumatic procedure, in which a needle is inserted through the dura to access the dural space. After the needle is withdrawn from the dural space, there can be a persistent “hole” in the dura. If this “hole” is large enough, CSF fluid can leak out and cause a drop in CSF pressure. It is believed that this drop in pressure decreases the fluid supporting the brain causing traction on the brain which cause the resultant headache.
LPs are a traumatic procedure, in which a needle is inserted through the dura to access the dural space. After the needle is withdrawn from the dural space, there can be a persistent “hole” in the dura. If this “hole” is large enough, CSF fluid can leak out and cause a drop in CSF pressure. It is believed that this drop in pressure decreases the fluid supporting the brain causing traction on the brain which cause the resultant headache.- It is also theorized that a drop in CSF volume will cause a direct activation of adenosine receptors. This activation leads to cerebral vasculature vasodilatation which can cause “cerebral stretching” and result in headaches.
What is the evidence for prevention of post LP headaches?
Needle Size: Size of the dural puncture site is directly proportional to the likelihood of headache development. Incidence of headache: [1]
 16 – 19G Needle ≈ 70%
16 – 19G Needle ≈ 70%- 20 – 22G Needle ≈ 40%
- 24 – 27G Needle ≈ 12%
Needle size must however be large enough to withdraw fluid safely, efficiently, and measure accurate opening pressures. Spinal needles < 22G may give false opening pressure readings and take as long as 6 minutes to withdraw 2mL of CSF, therefore the smallest recommended size needle for diagnostic and therapeutic LPs is 22G [2]
Direction of Needle Bevel: Dural fibers run in a top to bottom longitudinal direction, therefore, a needle bevel passing parallel to these fibers will just push them apart rather than lacerate them right? [3]:
 1021 lumbar punctures done
1021 lumbar punctures done- Perpendicular direction = 10.2% incidence of post LP headache
- Parallel direction = 5.5% incidence of post LP headache
- Conclusion: Parallel direction of needle bevel does decrease incidence of post LP headache
Stylet Replacement: Not replacing the stylet prior to spinal needle removal may cause increased post LP headache incidence. The theory is that a strand of arachnoid, which might enter the needle with the outflowing CSF during LP and upon removal of the needle, be threaded back through the dura to produce prolonged CSF leakage [4]:
 600 LPs performed
600 LPs performed- 300 had stylet replaced vs not replaced before withdrawal of spinal needle
- Incidence of post LP headache was 16% in the group not having stylet replaced vs 5% in group that did
- Conclusion: Replacement of stylet before spinal needle withdrawal, decreases incidence of post LP headache
Bed rest after LP: Does bed rest post LP decrease incidence of post LP headache? [5]
 Cochrane Review
Cochrane Review- 12 trials (1519 participants)
- No beneficial effect on incidence of post LP headache with bed rest vs immediate mobilization (26.4% vs 20.5%; RR 1.30)
- Conclusion: There is no difference in post LP headache incidence with early ambulation vs bed rest after LP
Also a systematic review looking at bed rest vs early ambulation of LP looking at OR of post LP headache showed [6]:
- Any headache (11 studies; 1693 patients) = OR 1.1
- Postural headache (8 studies; 1254 patients) = OR 1.2
- Severe postural headache (8 studies; 1342 patients) = OR 1.1
- Conclusion: Bed rest of any duration after LP does not decrease the incidence of post LP headache
Number of LP attempts: Pathophysiologically it makes sense that the more attempts made at LP the more likely a person is to suffer from post LP headaches. Since post-LP headaches are secondary to persistent CSF leaks, the more trauma caused by the provider, the more likely the patient is to leak CSF and suffer from headaches. What is the evidence?
- No studies to date have been conducted to compare one attempt versus multiple attempts [1]
Volume of CSF fluid removed: Is the volume of CSF removed a risk factor for headache after LP? [7]
- 501 LPs performed
- Questionnaire given to patients
- Mean CSF removal 12.9mL with no post LP headache vs 12.4mL with post LP headache (Not statistically significant)
- Conclusion: Volume of CSF was not a risk factor for post LP headache
Patient position: Does a sitting versus lateral decubitus position make a difference in incidence of post LP headache? [5]
- Cochrane Review
- 2 Trials with 120 patients
- No difference between positions regarding incidence of post LP headache (RR 0.86)
- Conclusion: The position that LP is performed does not make a difference in post LP headache
IVF prior to lumbar puncture: Does giving IVF prior to lumbar puncture decrease the incidence of post LP headache? [8]
- 100 patients having CT myelography performed
- 2 L of IVF 2 hours prior to procedure vs no IVF (RR 0.9)
- Conclusion: IVF prior to LP does not decrease incidence of post LP headache, but may decrease duration of headache > 24 hours.
What is the evidence for the treatments of post lumbar puncture headaches?
Early hydration following LP: Does administration of fluids after LP decrease incidence of post LP headache?
Only one study looked at this: [9]
- 100 patients having LP performed
- Patients asked to drink oral fluids 1.5L vs 3.0L post LP
- 64% had no post LP headache in both groups
- Limitation: Oral hydration post LP evaluated only
- Conclusion: Oral hydration post LP does not appear to decrease incidence of post LP headache
Caffeine: Does IV caffeine improve post LP headaches? [10] [11]
 IV caffeine given to 41 patients
IV caffeine given to 41 patients- Persistent headache at 1 – 2 hours post administration
- Absolute Risk Reduction of 0.68 (NNT 1.6)
- Limitation: High recurrence of headache (30%)
- Conclusion: IV caffeine 500mg provides a temporary improvement in symptoms for post LP headache
- One caveat: One cup of coffee contains about 50 – 100 mg of caffeine and soft drinks contain 35 – 50 mg
Prophylactic Blood Patch:
 It was noticed early on that patients with “traumatic taps” or “bloody taps” had a lower incidence of post-LP headaches. It has been theorized that this may be due to the patient’s own coagulation system helping form a patch over the hole created by the needle in the dura. Once the post-LP headache has already set in, a blood patch made by injecting 10-30 mLs of the patient’s blood into the epidural space can cause resolution of symptoms in 85-98% of cases if done in the first 24 hours [10]. This is likely due to the coagulating effect of the blood over dural compromise. It makes sense that using prophylactic blood patching immediately after finishing the procedure would help prevent post-LP headaches. However, the data is conflicting. This is likely due to the fact that the studies that have looked at prophylactic blood patching have limited the amount of blood used to 2-3 mLs, which may be insufficient. Data is very supportive of blood patching once the headache has set in.
It was noticed early on that patients with “traumatic taps” or “bloody taps” had a lower incidence of post-LP headaches. It has been theorized that this may be due to the patient’s own coagulation system helping form a patch over the hole created by the needle in the dura. Once the post-LP headache has already set in, a blood patch made by injecting 10-30 mLs of the patient’s blood into the epidural space can cause resolution of symptoms in 85-98% of cases if done in the first 24 hours [10]. This is likely due to the coagulating effect of the blood over dural compromise. It makes sense that using prophylactic blood patching immediately after finishing the procedure would help prevent post-LP headaches. However, the data is conflicting. This is likely due to the fact that the studies that have looked at prophylactic blood patching have limited the amount of blood used to 2-3 mLs, which may be insufficient. Data is very supportive of blood patching once the headache has set in.
Conclusion: A blood patch of at least 10 – 30mL is quite effective in treating post LP headaches
Take Home Messages
What Helps Prevent Post LP Headaches:
- 20 – 22G needles seems to be the optimal size for diagnostic/therapeutic LPs in adults
- Needle bevel parallel to dural fibers
- Replacement of stylet before withdrawal of spinal needle
- Early ambulation, NOT laying flat post procedure
- Number of LP attempts (Never studied, but pathophysiologically makes sense)
What DOES NOT Help Prevent Post LP Headaches:
- Volume of CSF removed
- Patient Position
- IVF prior to LP, but may decrease duration of headache being > 24 hours
Treatment:
- Oral hydration after lumbar puncture does not improve treatment (would like to see a study with IVF)
- The evidence is weak, but IV or oral caffeine does improve post LP headache, but with a high recurrence rate
- Blood patch is an effective treatment for post LP headache
References:
- Ahmed SV et al. Post Lumbar Puncture Headache: Diagnosis and Management. Postgrad Med J 2006. PMID: 17099089
- Carson D et al. Choosing the Best Needle for Diagnostic Lumbar Puncture. Neurology 1996. PMID: 8710120
- Lybecker H et al. Incidence and Prediction of Postdural Puncture Headache. A Prospective Study of 1021 Spinal Anesthesias. Anesthesiologists Analg 1990. PMID: 2316881
- Strupp M et al. Incidence of Post-Lumbar Puncture Syndrome Reduced by Reinserting the Stylet: A Randomized Prospective Study of 600 Patients. J Neurol 1998. PMID: 9758296
- Arevalo-Rodriguez I et al. Posture and Fluids for Preventing Post-Dural Puncture Headache. Cochrane Database Syst Rev 2013. PMID: 23846960
- Jacobus CH. Does Bed Rest Prevent Post-Lumbar Puncture Headache? Ann Emerg Med 2012. PMID: 21689866
- Kuntz KM et al. Post-Lumbar Puncture Headaches: Experience in 501 Consecutive Procedures. Neurology 1992. PMID: 1407567
- Eldevik OP et al. The Effect of Dehydration on the Side Effects of Metrizamide Myelography. Radiology 1978. PMID: 152937
- Dieterich M et al. Incidence of Post-Lumbar Puncture Headache is Independent of Daily Fluid Intake. Our Arch Psychiatry Neurol Sci 1988. PMID: 3203698
- Lin W et al. Myth: Fluids, Bed Rest, and Caffeine are Effective in Preventing and Treating Patients with Post-Lumbar Puncture Headache. West J Med 2002. PMID: 11788546
- Morley-Forster PK et al. The Effect of Epidural Needle Type on Postdural Puncture Headache: A Randomized Trial. Can J Anaesth 2006. PMID: 16738291
For More on This Topic Checkout:
- Ken Milne at The SGEM: SGEM#134 – Listen, to what the British Doctors Say about LPs post CT for SAH
- Rob Orman at ERCast: The Subarachnoid Enigma



