 So you are minding your own business when a 60 year old patient comes in after witnessed Out-Of-Hospital Cardiac Arrest (OHCA). She had a witnessed arrest, good bystander CPR and the prehospital team shocked her out of ventricular fibrillation (vfib), intubated her and brought her in after 25 min of total down time and 15 min of CPR. She is now neurologically stunned but with a stable blood pressure. You get an EKG which shows normal sinus rhythm with non-specific ST and T wave changes(NSR NSSTTW changes) basic labs, and are hunting for a source. Labs, chest x-ray (CXR), point of care ultrasound (POCUS) by you doesn’t reveal an alternate source to explain the arrest. You start hypothermic protocol and are thinking of sending her to the ICU. Or maybe not? What about the cath lab? Your resident recalls some early data from European studies cathing some of these patients that trended towards favorable results and wants to know how you do things here? The new ACC guidelines just published this month, July 2015 are here to answer that very question.
So you are minding your own business when a 60 year old patient comes in after witnessed Out-Of-Hospital Cardiac Arrest (OHCA). She had a witnessed arrest, good bystander CPR and the prehospital team shocked her out of ventricular fibrillation (vfib), intubated her and brought her in after 25 min of total down time and 15 min of CPR. She is now neurologically stunned but with a stable blood pressure. You get an EKG which shows normal sinus rhythm with non-specific ST and T wave changes(NSR NSSTTW changes) basic labs, and are hunting for a source. Labs, chest x-ray (CXR), point of care ultrasound (POCUS) by you doesn’t reveal an alternate source to explain the arrest. You start hypothermic protocol and are thinking of sending her to the ICU. Or maybe not? What about the cath lab? Your resident recalls some early data from European studies cathing some of these patients that trended towards favorable results and wants to know how you do things here? The new ACC guidelines just published this month, July 2015 are here to answer that very question.
What article are we referring to?
Rab et al. Cardiac Arrest: A Treatment Algorithm for Emergent Invasive Cardiac Procedures in the Resuscitated Comatose Patient. JACC July 2015. PMID: 26139060
Background:
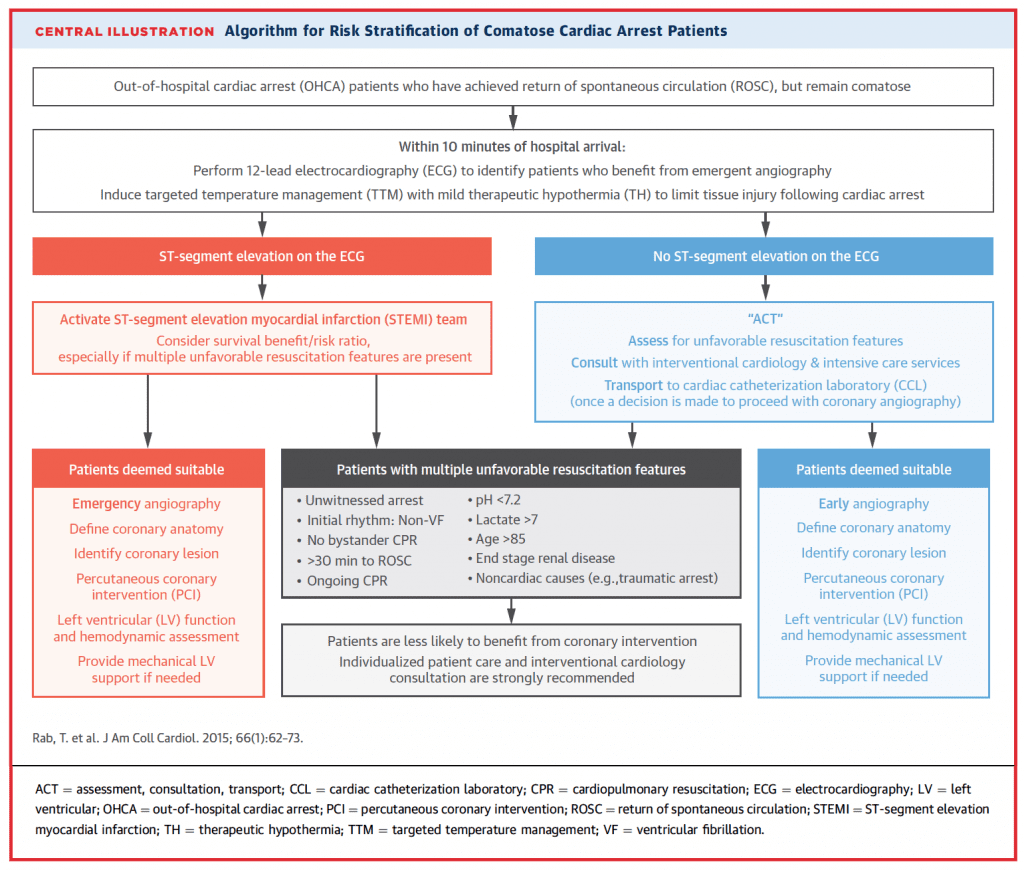
- EKG in post arrest patients within 10 min
- Early Target Temperature Management (TTM)
- Indications for Cath on post arrest patients
- A – Assess: for favorable and unfavorable resus features
- C – Consult: cardiology to determine the best strategies
- T – Transport: to a PCI center if your assessment and consultants favor an invasive strategy
Discussion:
Most resuscitationists will comply with early EKG and TTM, as well as, activate the cath lab for candidates with STEMI. There are several things to discuss regarding this document, some are good and some are bad, but one of the most practice changing recommendations is the decision to cath post arrest patients without STEMI. The authors list a set guidelines that can help guide our patient selection and decision to consult our cardiology colleagues to proceed with an early invasive strategy in the cath lab with hopes of favorable outcomes. First, lets go through the quick list of factors:
Unfavorable for Cath:
- Unwitnessed arrest: If ROSC and survival should be achieved in this scenario, the rate of favorable neurological outcome is less than in those with witnessed arrest [3]
- Initial non-VF Rhythm: Nonshockable rhythms are associated with worse outcomes as compared to shockable rhythms [3]
- Lack of bystander CPR: No early bystander CPR is associated with worse long-term outcomes (Survival = Bystander CPR 16.1% vs No Bystander CPR 3.9%) [4]
- >30 min to ROSC: Resuscitation efforts >30 minutes have worse survival and neurologic outcomes. Favorable (Cerebral Performance Category 1 0r 2) neurologic outcomes post-arrest were seen at 18 ± 15 min vs non-favorable (Cerebral Performance Category 3, 4, or 5) at 47 ± 18 min [5]
- >30 min of CPR: Duration of CPR has been shown to be an independent predictor of poorer functional status after OHCA [6]
- Evidence of unresponsive hypoperfusion and microcirculatory failure:
- pH <7.2 and Lactate >7: The PROCAT (Parisian Region Out of hospital Cardiac ArresT) Study showed that 112/264 non-survivors of cardiac arrest had a lactate >7mmol/L and a pH <7.2 in post cardiac arrest survivors indicates risk of left ventricular dysfunction and poor neurological recovery [7].
- Age >85: In a large registry of patients > 85 years of age after cardiac arrest, 60% did not achieve ROSC, and mortality was 90% [8]
- End-Stage Renal Disease (ESRD): Survival of ESRD patients after cardiac arrest is <15% after 1 year [9]
- Non-Cardiac Causes: Cardiac arrest due to drugs, drowning, acute stroke, terminal cancer and trauma, just to name a few non-cardiac causes, are likely to result in poor outcomes post-resuscitation.
Immediate Coronary Angiography in Patients Without STE on ECG?
The majority of patients with ROSC after cardiac arrest do not have STE on post-arrest ECG. Unfortunately, data supporting immediate coronary angiography in patients without STE, is not as clear as the evidence in patients with STEMI. The article states that approximately 1/4 of patients without STE have an acute occlusion and nearly 60% will have significant obstructive lesions (Table shown below).
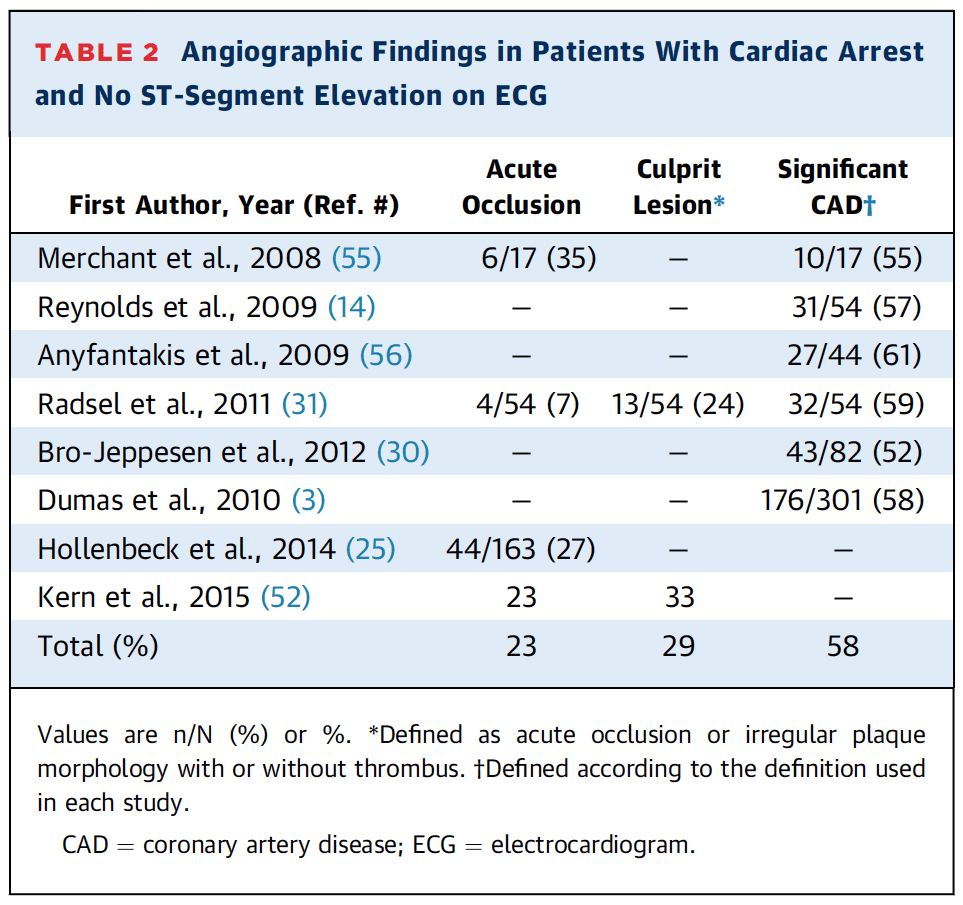
They go on to say that clinical and ECG characteristics are poor predictors of acutely occluded vessels and that coronary angiography should remain the “gold standard” for identification of culprit arteries. There was one study by Hollenbeck et al [10] which is the only study to look at an early invasive strategy and its effects on neuro outcomes in a group of patients with cardiac arrest who did not have STE on ECG. They found that an early invasive strategy was associated with a better long-term survival (60% vs 40.4% [p = 0.005]) and a more favorable neurological outcome (60.0% vs 39.7% [p = 0.004]).
Back to Our Patient:
Clinical Take Home Message:
Many patients with OHCA, even those without STE on initial ECG, will benefit from an early invasive strategy of TTM and coronary angiography, if we select the right patients and are aggressive in our resuscitation efforts.
- The majority of the studies cited are observational reports and retrospective registries. We should interpret these studies with caution. Observational studies can be confounded with other factors not taken into account (i.e. quality of CPR). At the end of the day, do we really need more excuses to not take people to angiography/PCI based off studies with limited numbers of patients and possible confounders?
- The old adage of treat the patient and not the numbers. I am not sure that making a blanket statement of “poor candidate” for cath/PCI with pH <7.2 and lactate >7 is appropriate. As a matter of fact, the lactate recommendation comes from an observational study of 26 patients. Is this really what we are going to use as evidence to determine a patients outcome? 26 patients? Most patients in cardiac arrest are going to have pH <7.2 and very elevated lactates, this is why we aggressively resuscitate them. As a matter fact there is an older paper by Schultz SC et al [11] that showed in cardiac arrest there is no correlation to survival and initial pH.
- Age alone should not be an exclusion criterion for angiography/PCI, but should be assessed in a case by case basis. We have all seen 80 year old patients who look like they are sixty something, with an excellent quality of life (i.e. physiological age vs true age). To make a generalization about age in my opinion is not appropriate.
- There are several factors that are listed as definitions of futility for angiography/PCI in OHCA. But, are we supposed to take this as the letter of the law? How many of these factors need to be present before withholding angiography/PCI? There are currently no established thresholds for what chance of a favorable outcome warrants aggressive treatment, and I suspect for everyone this will be different.
- In this day and age of ultrasound, I don’t see anywhere on the algorithm where bedside cardiac ultrasound to look at cardiac activity or wall motion abnormalities are used for decision making. A systematic review by Cohn et al [12] showed that the absence of cardiac activity on ultrasonography did not universally mean failure of resuscitation in cardiac arrest, but it did show that a survival rate was only 2.4% in patients with cardiac standstill. Ultrasound is quick and easy, and gives us prognostic information that could be useful in the decision making process of futility, not a random lactate or pH.
- The Hollenbeck et al [10] study is a retrospective, observational study of a prospective cohort of 754 consecutive comatose patients treated with therapeutic hypothermia (TH) following cardiac arrest. A total of 269 of these patients had cardiac arrest due to VF/VT without STEMI. Patients treated with early cardiac cath (defined as <24 hours), were more likely to survive to hospital discharge compared to those not treated with early cardiac cath (65.6% vs 48.6% p = 0.017). Interestingly, patients were even more likely to survive with early cardiac cath versus none at all (65.6 vs 28.6% p < 0.001). Now, of the patients who got early cardiac cath, regardless of whether they had PCI, similar survival rates with good neuro outcomes were seen (60% vs 62.2% p = 0.669), which argues that maybe its not the intervention of PCI, but “a greater intensity of care” in the early phase of hospitalization (i.e. mechanical support, anticoagulation, etc.).
- Finally, the bottom line here is, if you have a patient with OHCA and ROSC who is comatose, regardless of STE or non-STE on ECG we should activate the cath lab. We should not unilaterally make the decision to activate or not activate based on unfavorable resuscitation factors, but instead make this decision in conjunction with cardiology.
References:
- Rab T et al. Cardiac Arrest: A Treatment Algorithm for Emergent Invasive Cardiac Procedures in the Resuscitated Comatose Patient. JACC 2015. PMID: 26139060
- O’Gara PT et al. 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction: A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation 2013. PMID: 23247304
- Spaite DW et al. Statewide Regionalization of Postarrest Care for Out-of-Hospital Cardiac Arrest: Association with Survival and Neurologic Outcome. Ann Emerg Med 2014. PMID: 25064741
- Sasson C et al. Predictors of Survival from Out-of-Hospital Cardiac Arrest: A Systematic Review and Meta-Analysis. Circ Cardiovasc Qual Outcomes 2010. PMID: 20123673
- Komatsu T et al. Shorter Time Until Return of Spontaneous Circulation is the Only Independent Factor for a Good Neurological Outcome in Patients with Postcardiac Arrest Syndrome. Emerg Med J 2014. PMID: 23639589
- Reynolds JC et al. Duration of Resuscitation Efforts and Functional Outcome After Out-of-Hospital Cardiac Arrest: When Should we Change to Novel Therapies? Circulation 2013. PMID: 24243885
- Dumas F et al. Immediate Percutaneous Coronary Intervention is Associated with Better Survival After Out-of-Hospital Cardiac Arrest: Insights from the PROCAT (Parisian Region Out of hospital Cardiac ArresT) Registry. Circ Cardiovasc Interven 2010. PMID: 20484098
- Larkin GL et al. Pre-Resuscitation Factors Associated with Mortality in 49,130 Cases of In-Hospital Cardiac Arrest: A Report from the National Registry for Cardiopulmonary Resuscitation. Resuscitation 2010. PMID: 20047786
- Herzog CA. Cardiac Arrest in Dialysis Patients: Approaches to Alter an Abysmal Outcome. Kidney Int Suppl 2003. PMID: 12694343
- Hollenbeck RD et al. Early Cardiac Catheterization is Associated with Improved Survival in Comatose Survivors of Cardiac Arrest Without STEMI. Resuscitation 2014. PMID: 23927955
- Schultz SC et al. Predicting In-Hospital Mortality During Cardiopulmonary Resuscitation. Resuscitation 1996. PMID: 8959768
- Cohn B. Does the Absence of Cardiac Activity on Ultrasonography Predict Failed Resuscitation in Cardiac Arrest? Ann Emerg Med 2013. PMID: 23683545



