REBEL Cast Ep63 – LIDOKET – IV Lidocaine for Renal Colic?
The Article: Motov, Sergey, et al. “Comparing intravenous lidocaine/ketorolac combination to either analgesic alone for suspected renal colic pain in the ED.” The American Journal of Emergency Medicine (2019). [Epub Ahead of Print]
What They Did:
- Single-center, randomized double-blind trial of patients 18-64 with acute flank pain, abdominal pain, or back pain suspected to be due to renal colic by the treating ED physician and who warranted IV analgesia.
- Randomized to one of three groups:
- 1.5 mg/kg IV lidocaine given as 15-minute infusion
- 30 mg IV ketorolac
- 1.5 mg/kg IV lidocaine given as 15-minute infusion AND 30 mg IV ketorolac
- Rescue analgesia was offered as needed at 30 minutes and given as IV morphine, 0.1 mg/kg.
- Patients were evaluated at 15, 30, and 60 minutes.
- Excluded for age > 64 years, weight >100kg, pregnant or breastfeeding, contraindications to NSAIDs or lidocaine, known renal or hepatic dysfunction, use of NSAIDs or opioids within 4 hours, altered mental status, use of anticoagulants, and HR <50 or >150.
Outcomes:
- Primary: Pain reduction between groups at 30 minutes.
- Secondary:
- Comparative pain reduction between groups at 30 and 60 minutes.
- Need for rescue analgesia at 30 and 60 minutes.
Results:
- 150 total patients recruited (50 patients per group).
- Comparative pain reduction at 30 minutes:

- At 60 minutes:
![]()
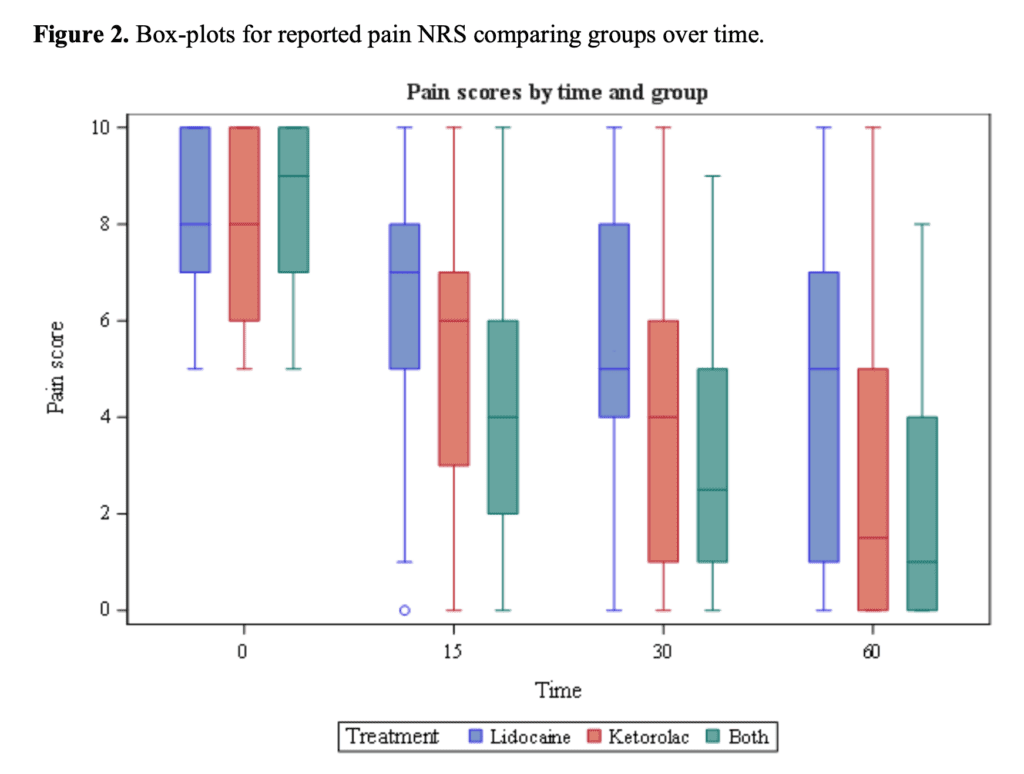
- ALL groups demonstrated pain reduction at 30 minutes, however both the lidocaine/ketorolac combination and ketorolac groups had larger changes in pain score than the lidocaine group at 30min post-administration
- NO CLINICAL DIFFERENCE in mean pain scores at all time points between lidocaine/ketorolac combination and ketorolac alone
- No statistical difference in rescue medication between groups, though a trend toward more morphine rescue analgesia in lidocaine-containing groups (14% in the lidocaine group, 8% combination group, 6% ketorolac group).
- HIGHER RATES OF ADVERSE EVENTS among groups receiving lidocaine
- Any adverse effect
- 15 minutes: 32% lidocaine-containing groups vs 14% ketorolac alone.
- 30 minutes: 25% lidocaine-containing groups vs 6% ketorolac alone.
- 60 minutes: 20% lidocaine-containing groups vs 6% ketorolac alone.
- Most common adverse events with lidocaine were dizziness and nausea/vomiting.
- Any adverse effect
- In patients with confirmed renal colic, ketorolac alone and combination medication were superior in pain reduction compared to lidocaine alone in subgroup analysis.
Figure 1. Box plot for reported pain scores over time.
Strengths:
- Narrowly-defined clinical question applied pragmatically.
- Baseline pain was similar between groups (i.e. ≈8 on mean NRS).
- Addresses the role of lidocaine in the setting of common practice (ketorolac co-administration).
- All randomized patients available for pre-specified outcome data.
- Thorough adverse effect observation and reporting.
- Preparing pharmacist, research manager and statistician were the only members of the team with knowledge of the study arm to which the participant was randomized, leaving providers, participants, and data collecting research team blinded to the medication received,
Limitations:
- Convenience sample compounds selection bias, suggested by time for recruitment of nearly two years.
- Small sample size of 150 subjects inadequate to assess variance in safety of the 3 different study medications, though the higher incidence of adverse events in patients receiving IV lidocaine is likely accurate.
- Patients with suspected renal colic were included, and 40% of total patients received alternate diagnoses at discharge (flank pain, UTI/pyelonephritis, etc.). Isolation to a cohort with diagnosed renal colic may lead to different results.
- Patients were only followed for 60 minutes, and thus subsequent events are unknown (i.e. rates of discharge vs admission, bouncebacks, etc.).
Author Conclusion:
- “Administration of an IV lidocaine/ketorolac combination to ED patients with suspected or documented renal colic results in better analgesia in comparison to parenteral lidocaine alone but provides no analgesic advantages over parenteral ketorolac alone.”
REBEL Commentary:
- Previous trials have not included (or not reported) routine use of ketorolac or other NSAIDs for treatment of renal colic, severely limiting applicability, as NSAIDs are part of the typical ED management of renal colic.
- Adoption of IV lidocaine for the treatment of renal colic in the ED outpaced literature supporting its use, likely driven by a desire to limit opioid exposure and identify alternative effective analgesics.
Clinical Take Home Point:
- The addition of lidocaine to ketorolac for the treatment of suspected renal colic has no clinical benefit, but may result in increased adverse events.
- Lidocaine should not be recommended for routine widespread use for treatment of renal colic in the ED.
References:
- Soleimanpour, Hassan, et al. “Effectiveness of intravenous lidocaine versus intravenous morphine for patients with renal colic in the emergency department.” BMC urology1 (2012): 13. PMCID: 3508963
- Firouzian, Abolfazl, et al. “Does lidocaine as an adjuvant to morphine improve pain relief in patients presenting to the ED with acute renal colic? A double-blind, randomized controlled trial.” The American journal of emergency medicine3 (2016): 443-448. PMID: 26704774
- Motamed, Hassan, and Mohammadreza Maleki Verki. “Intravenous Lidocaine Compared to Fentanyl in Renal Colic Pain Management; a Randomized Clinical Trial.” Emergency1 (2017). PMCID: 5703759
- Fitzpatrick, Brendan Michael, and Michael Eugene Mullins. “Intravenous lidocaine for the treatment of acute pain in the emergency department.” Clinical and experimental emergency medicine2 (2016): 105. PMCID: 5051607
Post Peer Reviewed By: Anand Swaminathan, MD (Twitter: @EMSwami), Mizuho Morrison, DO (Twitter: @mizspangler), and Salim R. Rezaie, MD (Twitter: @srrezaie)



