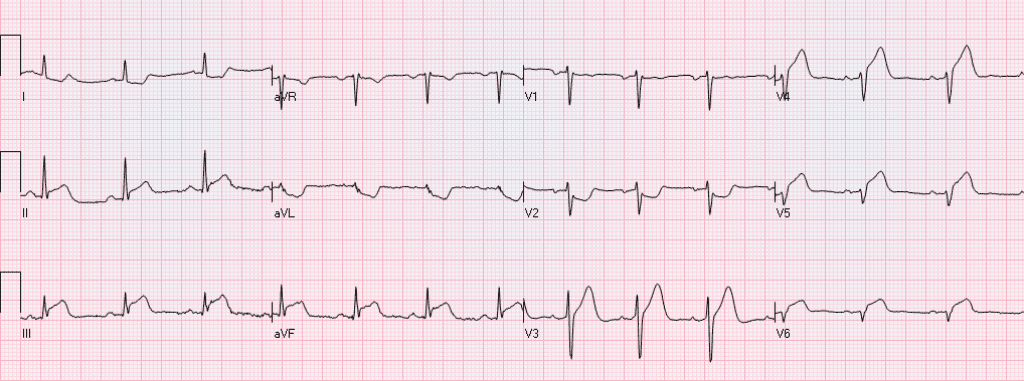
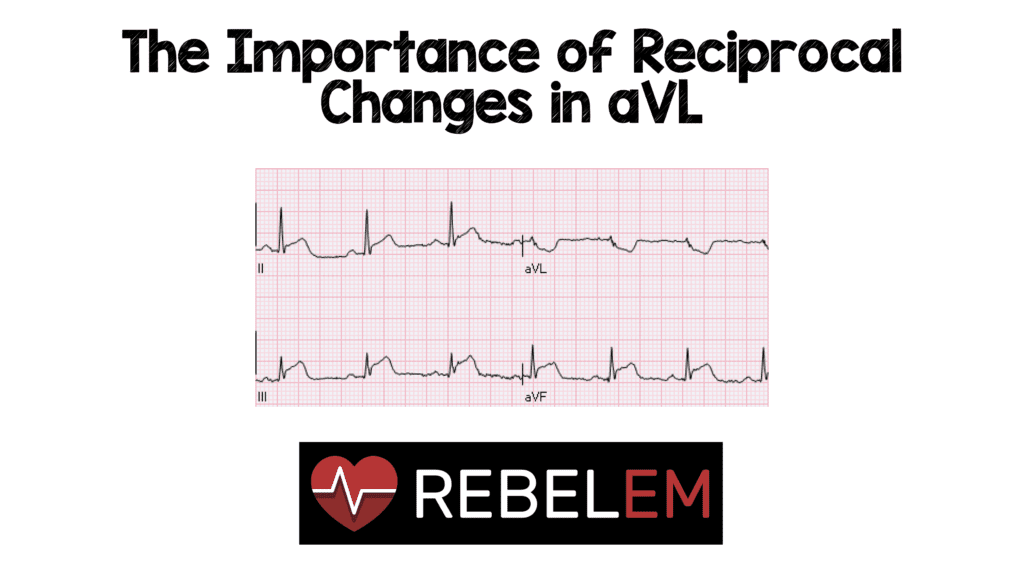
 ECG interpretation is one of the most important skills to master as an emergency physician, and its interpretation can be very complex and frustrating. ECG manifestations can be very subtle, and sometimes the earliest and only ECG change seen will be reciprocal changes alone. To further complicate this, many patients have the atypical symptoms of nausea/vomiting, weakness, or shortness of breath and not chest pain.
ECG interpretation is one of the most important skills to master as an emergency physician, and its interpretation can be very complex and frustrating. ECG manifestations can be very subtle, and sometimes the earliest and only ECG change seen will be reciprocal changes alone. To further complicate this, many patients have the atypical symptoms of nausea/vomiting, weakness, or shortness of breath and not chest pain.
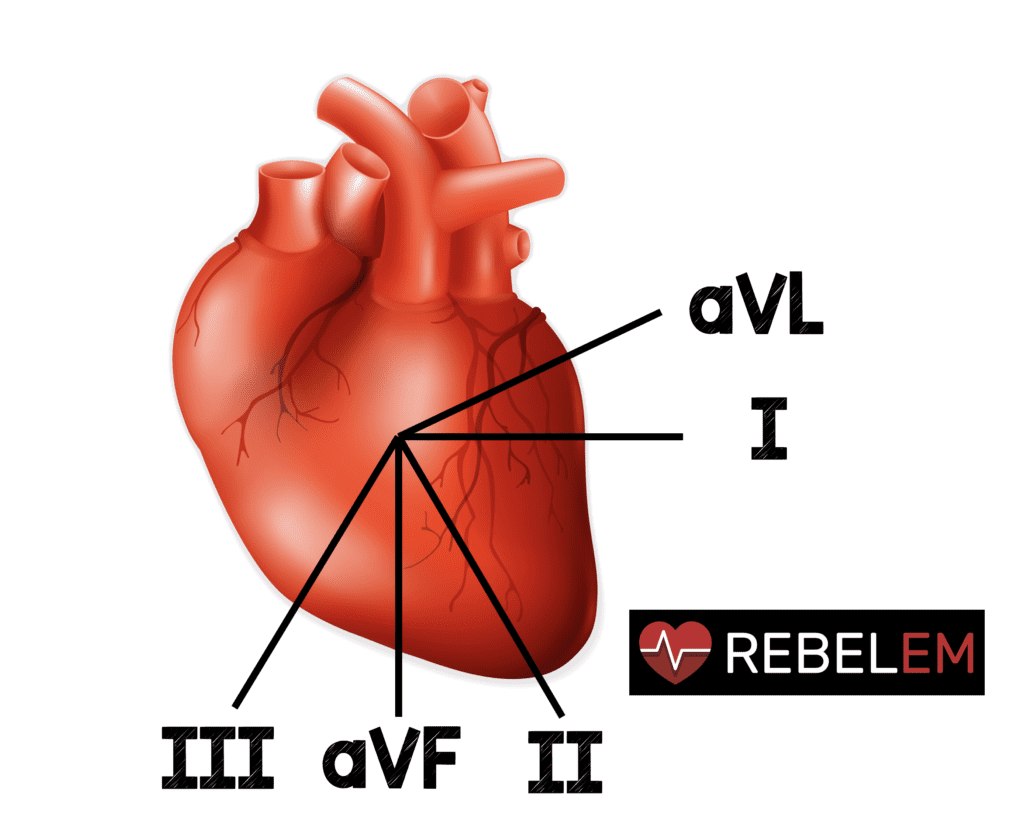 What is the anatomic location of aVL to the heart?
What is the anatomic location of aVL to the heart?
- aVL is the only lead facing the superior part of the left ventricle
- aVL is the only lead that is opposite the inferior wall of the heart (almost 180 degrees from lead III)
What is the differential diagnosis for reciprocal changes in aVL?
- Inferior acute myocardial infarction
- Anterior acute myocardial infarction
- Left ventricular hypertrophy
- Left bundle branch block
- Digitalis Use
How good are reciprocal changes in aVL in diagnosing myocardial infarction (MI)?
- 53.3% of patients with inferior wall MI had reciprocal changes ≥ ST elevation in inferior leads [1]
- 70 – 97.2% of patients with inferior wall MI had reciprocal changes in aVL [2] [3]
- 30% of patients with anterior wall MI had reciprocal changes in aVL [3]
Can lead aVL give prognostic information for acute MI?
ST depression ≥0.1 mV in 2 or more lateral leads (I, aVL, V5, or V6) are more likely to:
- Die (14.9% vs 4.1%) [4]
- Suffer severe heart failure (14.3% vs 4.1%) [4]
- Have angina with ECG changes (20.0% vs 11.6%) [4]
What is the most likely culprit artery in inferior MI?
- Right coronary artery (80% of cases): Most likely especially if:
- ST segment elevation lead III > lead II and ST segment depression in lead I and aVL (> 1 mm)
- Sens 90%, Spec 71%, PPV 94%, and NPV 70%) [5]
- Left circumflex artery (20% of cases)
Conclusion
Reading of the ECG remains a crucial diagnostic and prognostic tool for acute MI, and the earliest finding of an acute MI may be reciprocal changes in lead aVL.
References:
- Parale GP et al. Importance of Reciprocal Leads in acute Myocardial Infarction. J Assoc Physicians India 2004. PMID: 15656026
- Birnbaum Y et al. ST Segment Depression in aVL: A Sensitive Marker for Acute Inferior Myocardial Infarction. Eur Heart J 1993. PMID: 8432289
- Morris F et al. ABC of Clinical Electrocardiography. Acute Myocardial Infarction Part 1. BMJ 2002. PMID: 11934778
- Barrabes JA et al. Prognostic Significance of ST Segment Depression in Lateral Leads I, aVL, V5 and V6 on Admission Electrocardiogram in Patients with a First Acute Myocardial Infarction Without ST Segment Elevation. JACC 2000. PMID: 10841229
- Use of the Electrocardiogram in Acute Myocardial Infarction. NEJM 2003. PMID: 12621138
Cite this article as: Salim Rezaie, "The Importance of Reciprocal Changes in aVL", REBEL EM blog, November 1, 2013. Available at: https://rebelem.com/importance-reciprocal-changes-avl/.